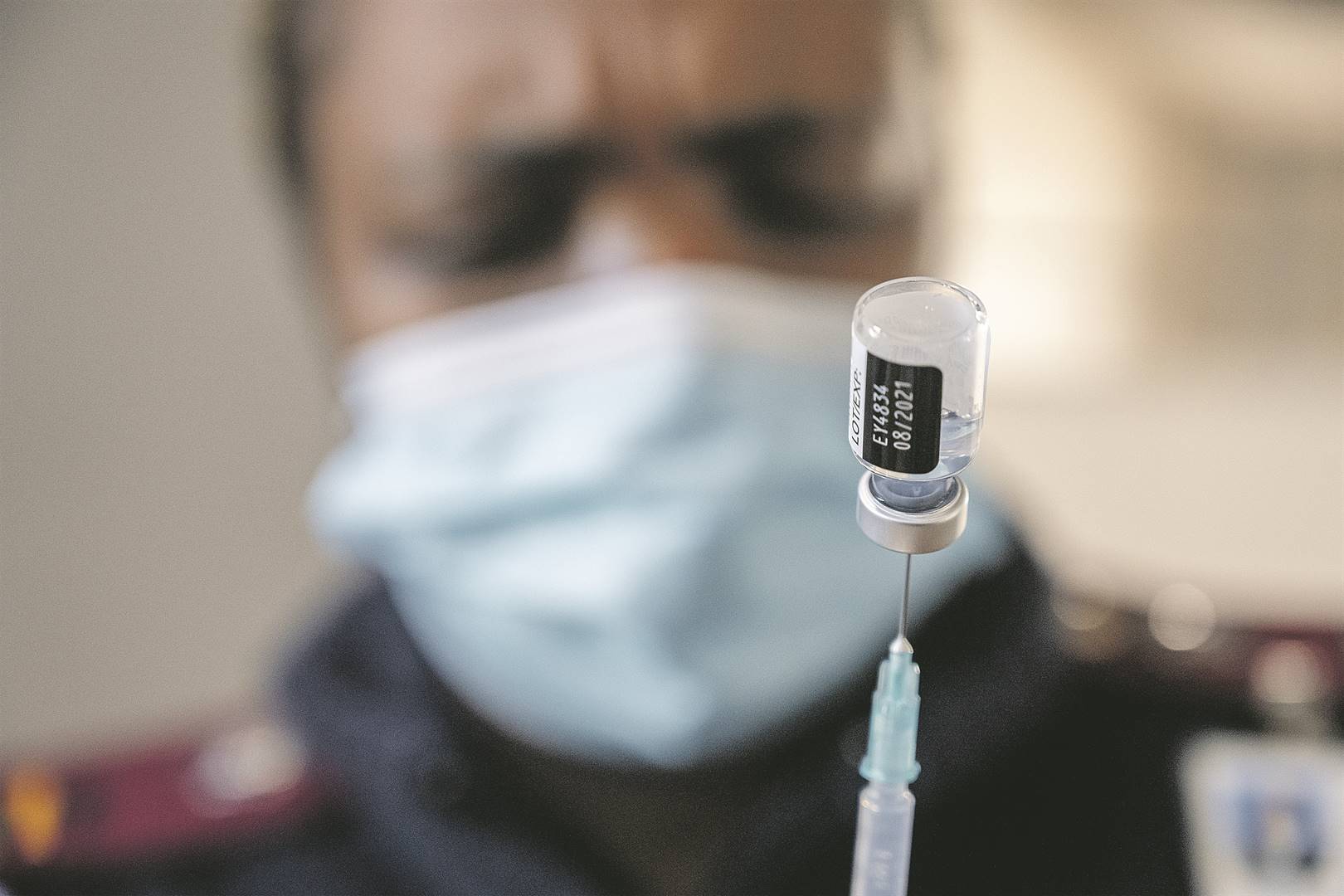
- South Africa has no budget for pandemics, it has emerged at a pandemic preparedness webinar.
- The head of the secretariat of the African Union Commission on Covid-19 said this was concerning.
- South African Medical Research Council president and CEO, Professor Glenda Gray, says non-communicable diseases kill more than 41 million people yearly.
Just months after the World Health Organisation (WHO) declared that the Covid-19 pandemic had ended, it has emerged South Africa does not have a budget for pandemics.
The information was revealed during the Pillar 10: Pandemic Preparedness Plan webinar on Friday, which the Presidency hosted in partnership with the Department of Health and WHO South Africa.
During the discusssion on considerations for future pandemics, head of the secretariat of the African Union Commission on Covid-19, Dr Lwazi Manzi, said it was concerning that South Africa did not have separate funds for pandemic prevention, preparedness and response (PPR).
She said the situation could be problematic in the event of another pandemic in the future.
In May, the WHO declared an end to the Covid-19 pandemic.
In South Africa, the first pandemic-related loss of life occurred in March 2020. In that month, a countrywide lockdown was put in place as experts and government officials tried to get their heads around the disease and how to curb its spread.
The lockdown continued, at various levels of intensity, for roughly two years.
But the economic losses were dire.
READ | SA's disease burden placing strain on public health system - Phaahla
In 2019, President Cyril Ramaphosa launched the Presidential Health Compact, which introduced a five-year roadmap for health systems strengthening reforms under the "10 pillars" towards accelerating universal health coverage (UHC) in South Africa.
The pillars are:
- human resources;
- access to medicine, vaccines and health products;
- infrastructure;
- private sector engagement;
- quality healthcare;
- public sector financial management improvements;
- governance and leadership;
- community engagements; and
- information systems and pandemic preparedness.
These pillars were under discussion during Friday's webinar.
One of the speakers, South African Medical Research Council president and CEO, Professor Glenda Gray, said non-communicable diseases (NCD) killed more than 41 million people yearly. She said 80% of NCD deaths were the result of four diseases: type 2 diabetes, cancer, respiratory infections and cardiovascular diseases.
Gray said:
Gray said 10 million people were infected with tuberculosis (TB) annually.
Despite being preventable and curable, 1.5 million people die from TB yearly, making it the world's top infectious killer.
SATURDAY PROFILE | Progressive Health Forum's Dr Aslam Dasoo: 'Ramaphosa's intervention saw SA getting vaccines'
Gray added that TB was the leading cause of death for people diagnosed with HIV and a major contributor to antimicrobial resistance.
She added that there was a need to invest in science.
"There is a critical need to know who is born and dying, where and at what age. The National Health Laboratory Service footprint should also be maintained," she said.
Professor Salim Abdool Karim, the special advisor on pandemics to the director-general of the WHO said there was a need for decisive political leadership to be open to scientific advice.
ANALYSIS | HIV remains a leading killer in Africa despite breakthroughs – how to eliminate it
"There should be a pandemic preparedness plan for surveillance and epidemic intelligence. It is also important to look at medical countermeasures, especially diagnostic, vaccines, therapeutics, and respiratory devices. There is a need for a fit-for-purpose legal and financing framework with legal provisions for testing, quarantine, surveillance, disinformation control, border control, vaccination and financial controls to reduce corruption," Karim said.
Dr Owen Kaluwa, the WHO country representative, said the WHO developed a new organising framework to guide country pandemic preparedness planning for respiratory pathogens.
Kaluwa said:
He said the WHO supported the department and stakeholders in rolling out the integrated disease surveillance response.
Kaluwa added that the WHO would continue to provide technical support for other universal health coverage priorities, including the National Health Insurance, that are critical for the health system.
The panel said there was a need to build collaboration mechanisms and agreements between the public and private sectors.
"There is a need to strengthen the international health regulation processes in South Africa, communicate the work done with the broader group, build institutional capacity for surveillance, and improve laboratory and genomic-specific capacity at a periphery level in all provinces. Lab testing is also necessary to detect new variants through timeous and efficient sampling and testing and transport of samples."




 Publications
Publications
 Partners
Partners
























